Phone: +44 (0)20 8492 1600
Need help or have a question?
Contact us at: [email protected]
If you are one of the millions of people in the UK living with heel pain, this ultimate guide to plantar fasciitis covers everything you need to know, from causes and symptoms to the best treatments available in 2026. With NHS podiatry wait times projected to reach an average of 78 weeks by the end of 2026, understanding how to manage this condition at home, without delay, has never been more important for UK patients.
| Question | Quick Answer |
|---|---|
| What is plantar fasciitis? | It is an inflammation of the plantar fascia, a fibrous band of tissue connecting your heel to your toes, causing heel and arch pain. |
| What are the main symptoms? | Sharp heel pain, especially in the morning or after rest, plus tenderness under the arch of the foot. |
| What causes plantar fasciitis? | Overuse, poor footwear, flat feet, high arches, obesity, and spending long periods on hard floors are common triggers. |
| How do UK patients treat plantar fasciitis? | Supportive insoles and orthotics, stretching, rest, protective padding, and (in some cases) physical therapy are the most recommended approaches. Visit our plantar fasciitis guide for a full breakdown. |
| Do insoles really help? | Yes. Arch-supporting insoles and orthotics are one of the most widely recommended first-line treatments. Browse our plantar fasciitis products to find the right fit for you. |
| Is surgery needed? | Fewer than 10% of cases require surgery. It is only considered after 6 to 12 months of failed conservative care. |
| How long does plantar fasciitis last? | With proper management, many patients see improvement within a few months, though around 40% still report symptoms two years later if not consistently treated. |
Plantar fasciitis is one of the most common causes of heel pain in the UK, affecting people of all ages, fitness levels, and walks of life. The condition occurs when the plantar fascia, a thick band of fibrous tissue running along the bottom of your foot from your heel bone to your toes, becomes irritated and inflamed.
Think of the plantar fascia as the natural shock absorber of your foot. When it is placed under repeated stress or strain, tiny tears can develop, triggering pain and inflammation that makes everyday activities like walking to the kitchen, climbing stairs, or standing at work feel far harder than they should.

Your feet are your connection with the world, and when heel pain takes hold, it affects everything. That is why we at Profoot believe in giving UK patients clear, practical information so they can get back on their feet as quickly as possible.
Plantar fasciitis does not usually appear overnight. It tends to build up gradually as a result of repeated stress on the heel and arch, and several specific factors make certain people more likely to develop it.
The most common causes include:
There has been a 42% increase in what health professionals are calling “WFH Foot” conditions since 2024, largely because people are walking barefoot on hard floors at home and sitting at poorly set-up workstations. If you work from home, this is a pattern worth paying close attention to.
The symptoms of plantar fasciitis are quite distinctive, which makes it possible for many people to identify the condition before they visit a professional. The most telling sign is a sharp, stabbing pain on the underside of the heel, particularly when you take your first steps in the morning.
Other common symptoms include:
Did You Know?
94% of plantar fasciitis sufferers experience the most intense pain during their first few steps in the morning.
Source: NIH / PubMed Central
That classic morning pain is the hallmark symptom that helps distinguish plantar fasciitis from other heel conditions like heel spurs or Achilles tendinopathy. If you recognise that pattern, you are very likely dealing with plantar fasciitis.
It is worth noting that only 32% of UK adults experiencing foot pain received a formal diagnosis in 2025, meaning a large number of people are trying to manage heel pain without knowing exactly what they are dealing with. Getting a proper assessment from a GP, podiatrist, or physiotherapist makes a real difference to recovery outcomes.
Plantar fasciitis can affect anyone, but certain groups face a noticeably higher risk. Understanding your personal risk factors is the first step to prevention and early management.
Age: The condition is most common in adults between 40 and 60, as the plantar fascia naturally loses elasticity with age.
Runners and high-mileage athletes: Runners who exceed 40km (approximately 25 miles) per week face a six times higher risk of developing plantar fasciitis compared to those with moderate training loads. If you are part of the UK’s large running community, keeping an eye on your weekly mileage is genuinely useful.
People who stand for long periods: Teachers, nurses, retail workers, and factory staff are all at elevated risk due to prolonged standing on hard surfaces.
Those with foot mechanics issues: Flat feet, high arches, and overpronation all alter the distribution of weight across the foot, making the plantar fascia work harder than it should.
People carrying excess weight: Greater body mass means greater impact load on the heel with each step, accelerating wear on the fascia.
Visiting our common foot problems section gives you a broader picture of foot conditions that often accompany plantar fasciitis, including corns, calluses, and arch issues.
A GP or podiatrist will usually diagnose plantar fasciitis through a physical examination, reviewing your symptoms and pressing on specific areas of your foot to identify the source of pain. Imaging tests like X-rays or MRI scans are rarely needed unless another condition is suspected.
Because NHS podiatry waiting lists are so lengthy in 2026, many UK patients are choosing to self-assess using symptom checklists and begin conservative home treatment while waiting for an appointment. This approach is widely supported by UK healthcare professionals, provided you are using the right products and techniques.
Our foot care tips section offers practical, professional guidance you can put into practice straight away, so you do not have to wait weeks to start feeling better.
The good news is that the vast majority of plantar fasciitis cases respond well to conservative, non-surgical treatment. Fewer than 10% of patients ever need surgery, which is only considered after 6 to 12 months of persistent, failed conservative care.
The most effective treatment plan for UK patients typically combines several approaches:
Physical therapy was rated the most effective treatment for heel pain in 2025, outperforming over-the-counter medications, yet the NHS waiting list situation means many UK patients cannot access it quickly. Starting with high-quality insoles and protective padding from home is the most practical way to get pain relief while you wait.
You can read our dedicated article on insoles for plantar fasciitis for a detailed comparison of which products work best for different foot types.
Choosing the right insole can feel overwhelming, but the key features to look for are a deep heel cup, solid arch support, and shock-absorbing cushioning. We have put together a range of products specifically designed to meet those requirements for plantar fasciitis sufferers.
Did You Know?
83.2% of plantar fasciitis patients are found to wear ‘inappropriate’ footwear, such as shoes with minimal heel height or hard, non-cushioned soles.
Source: NIH / PubMed
Our 3-Zone Orthotics are one of our most popular choices for plantar fasciitis relief, and it is easy to see why. They feature a moulded design that supports the arch from front to back and side to side, with three distinct zones covering the heel, arch, and ball of the foot.
The three-quarter length design means they fit neatly into most styles of footwear without needing to remove your existing insole. They also come with our 30-day money-back guarantee, so you can try them with complete confidence.


The Heel and Arch Support Pain Relief Orthotics are designed specifically to ease the discomfort of plantar fasciitis, as well as associated knee and back pain caused by altered gait. The moulded design includes a built-in heel cup that provides targeted cushioning and shock absorption exactly where plantar fasciitis sufferers need it most.
They are also an excellent option for people who overpronate, as the arch support helps correct foot alignment during walking and standing.

If your plantar fasciitis pain is concentrated in the heel rather than the arch, our Gel Max Heel Cushions are an excellent targeted option. They feature an extra-thick PORON centre that delivers superior shock absorption and lasting cushioning throughout the day.
They are also designed to prevent the build-up of hard skin on the heel, which is a welcome added benefit for anyone managing chronic heel pain.

Browse our full insoles collection to compare all available options and find the right fit for your foot type and lifestyle.
| Product | Best For | Key Feature |
|---|---|---|
| 3-Zone Orthotics | All-round arch and heel support | Three-zone moulded design, 30-day guarantee |
| Heel & Arch Support Orthotics | Pronation and fascia strain | Deep heel cup, shock-absorbing moulded base |
| Gel Max Heel Cushions | Focused heel pain and hard skin | Extra-thick PORON centre, anti-fatigue design |
Alongside insoles and orthotics, protective padding plays a practical role in managing plantar fasciitis day to day. Padding helps to offload pressure from painful areas and reduce friction inside your footwear, giving your fascia more chance to recover.
Our Chiropody Felt is a professional-grade, self-adhesive padding used by chiropodists worldwide. You can cut it to shape and apply it directly inside your shoe or onto the skin to provide instant pressure relief around the heel and arch.
It is particularly useful for plantar fasciitis patients who need to customise the amount of padding in a specific spot, as every foot and every pain pattern is slightly different.

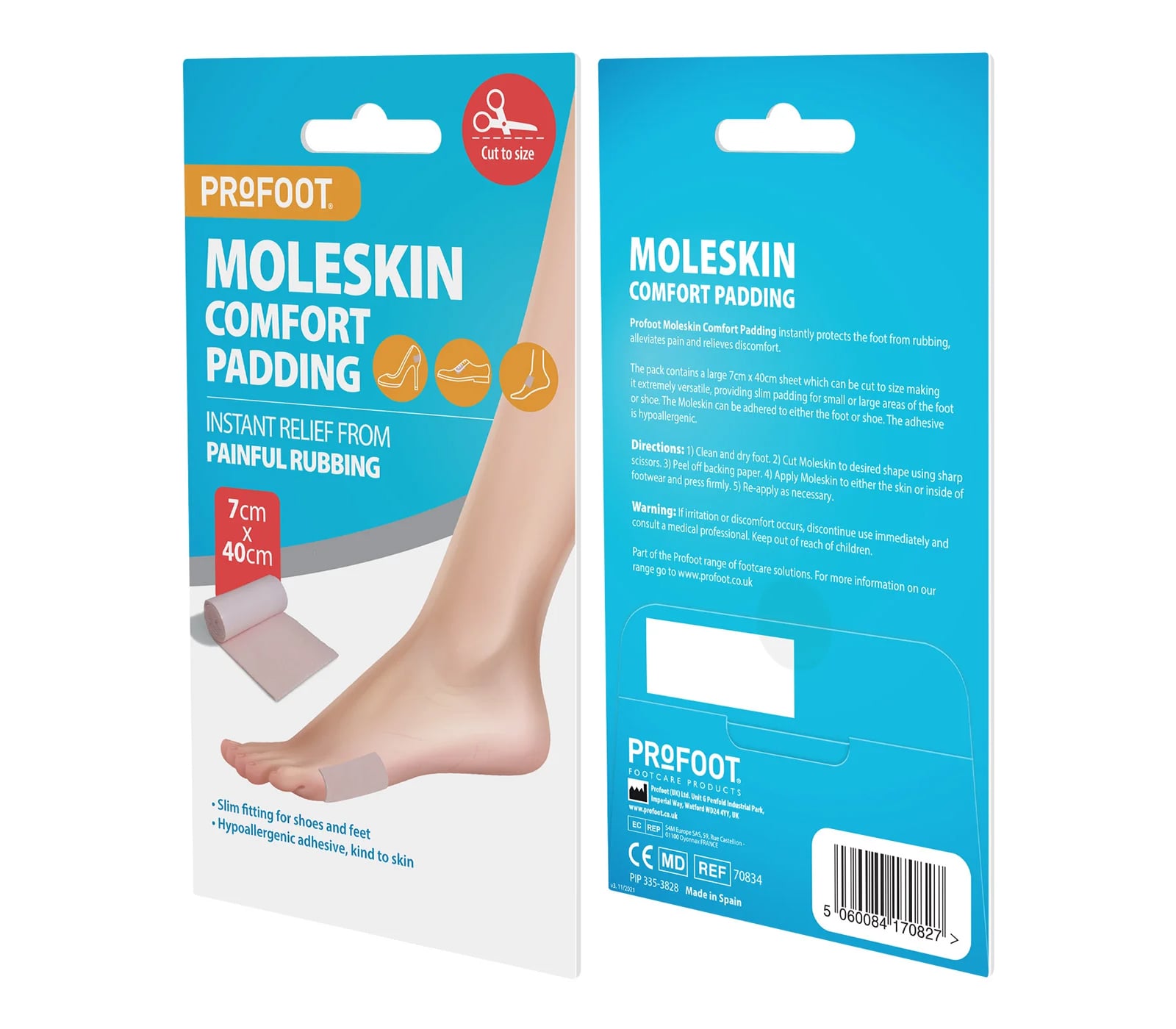
The Moleskin Roll is a generously sized (7cm x 40cm) hypo-allergenic padding roll that you can cut to size and apply wherever you need friction relief. It works well for plantar fasciitis patients dealing with additional irritation from footwear rubbing against already-tender areas.
Explore our full padding and protection products range to see everything available for managing plantar fasciitis discomfort at home.
88% of UK healthcare professionals now prioritise strengthening exercises over passive treatments like ultrasound for plantar heel pain. This means that when you visit a GP or podiatrist in 2026, they are very likely to give you a set of exercises to perform at home as part of your recovery plan.
The most effective stretches and exercises for plantar fasciitis include:
A foot massage ball is an excellent tool to have at your desk or beside your chair, as it lets you work on fascia mobility throughout the day without needing to stop what you are doing.
Footwear is arguably the single most controllable factor in managing and preventing plantar fasciitis. Poor shoe choices contribute to more than 83% of cases, yet switching to the right footwear can make a dramatic difference in a matter of weeks.
Look for shoes with:
Avoid:
Adding a quality insole to an otherwise supportive shoe can compensate for any lack of built-in arch support, making our 3-Zone Orthotics a smart pairing with your existing footwear.
Most cases of plantar fasciitis respond well to home management within a few weeks to months. That said, there are situations where seeing a professional promptly is the right move.
Book an appointment with your GP or podiatrist if:
Around 40% of patients still report symptoms two years after starting a traditional treatment protocol, which shows that plantar fasciitis is not always the self-resolving condition it is sometimes described as. Consistent, combined treatment (insoles, stretching, correct footwear, and professional input where needed) gives you the best long-term outcome.
Use our pharmacy finder to locate a stockist near you so you can get the right products quickly, without waiting for a delivery.
Once you have managed to get your plantar fasciitis under control, the last thing you want is for it to return. The good news is that with a few consistent habits, recurrence is very manageable.
Key prevention habits include:
Whether you have heel pain right now or you want to protect against it in the future, our full range of foot care products has everything you need to keep your feet comfortable and supported every single day.
This ultimate guide to plantar fasciitis for UK patients covers everything from understanding what causes the condition and recognising its symptoms, to finding the most effective treatments and prevention strategies available in 2026. The most important takeaway is this: you do not have to wait weeks on an NHS list before you start feeling better.
With the right insoles, protective padding, targeted stretches, and supportive footwear, most plantar fasciitis cases can be managed effectively at home. Our full range of plantar fasciitis products has been developed by foot care experts with over 20 years of family experience in helping people across the UK get back on their feet.
Your feet carry you through everything, and they deserve proper support. Whether you are waking up with that sharp morning heel pain for the first time or you have been managing plantar fasciitis for months, we are here to help. Feet have never felt so good, and with the right care, yours will not either.
“Whether you have heel, arch or ball of foot discomfort, Profoot have a solution for you. So you can keep moving, pain-free.”